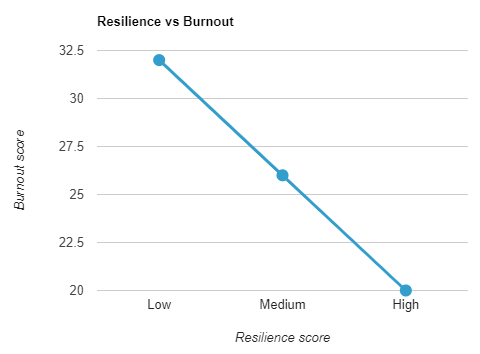
Wouldn’t it be awesome if the graph of physician resilience and burnout was a straight descending line? So, we just boost everyone’s resilience, burnout decreases, and everyone’s happy. Excellent!
Except, as always with us physicians, it’s complicated. Let’s look into this in a bit more detail.
Intuitively, yes. And there is some data supporting this position. But it’s always more complex when dealing with human beings, especially those of the doctor variety. It turns out that even our most resilient colleagues can burn out too.
Recent evidence (from during the pandemic) suggests that nearly 30% of physicians with the highest possible level of resilience still experience burnout.
I’m referring to a paper in JAMA Network Open written by Colin P West MB PhD from the Mayo Clinic and colleagues (2020). It was based on data collected in a nationwide US survey from >5,000 physicians and similar numbers of the general working population.
The authors used the Connor-Davidson Resilience Scale to measure resilience (range 0-8, with higher scores indicating higher levels of resilience) and the well-known Maslach Burnout Inventory, which includes measures for emotional exhaustion and depersonalization, to measure burnout.
Key findings:
Interestingly, resilience scores varied by medical specialty. (Let’s not get into which specialty attracts the wisest, brightest or strongest! Remember, these are average figures.)
Nevertheless, the highest resilience scores were found in physicians working in:
The lowest resilience scores were found in physicians working in:
My interpretation is that we medics are a resilient group, yet enhancing resilience is no guarantee against burnout.
Everyone has their breaking point.
And resilience training, while well-intentioned, can be counter-productive because it diverts attention from the underlying causes of physician burnout (as I have previously written about below).
For example, organizational “targets for improvement” may unintentionally worsen inefficiency, increase excessive workloads, and lead to negative leadership behaviors. Tackling the issues that cause physicians the most stress are are far more effective than individual-focused solutions such as those oriented around personal resilience.
The study’s main author, Dr West, states it clearly in a linked article: “Resilience training should not be the mainstay of responses to prevent burnout and promote well-being. Maintaining resilience is still important, but we need to look more to the work environment for solutions to burnout, as individual limitations are not driving physician distress and focusing on them may even be seen as a form of ‘victim-blaming.”
A narrow focus on increasing personal resilience is simply inadequate, and potentially dangerous, if we genuinely seek to address the epidemic of physician burnout.
...we are a resilient group, yet enhancing resilience is no guarantee against burnout. Everyone has their breaking point.
In that intersecting Venn diagram of resilience programs, peer-support, and collective agency lies Physicians Anonymous. Together we can address the complex and treatment-resistant root causes of burnout, while becoming stronger and happier by mutual support and understanding.
Our vision at Physicians Anonymous is to address the epidemic (pandemic?) of physician burnout, mental illness, addiction, and suicide.
We started up during the Pandemic after many years pre-Covid of offering informal peer support in our local hospitals. Covid made us realize that we needed to scale up by going online, ensure safety and anonymity, and reduce barriers to entry.
We wanted to make it easier for colleagues to come into the virtual rooms and feel safe to share among peers.
We hope that by providing safe, anonymous, online spaces where physicians can share in complete confidence, we will start to tackle this huge problem without victim-blaming.
Just doctors supporting doctors.
If the idea of a peer support group in a safe space is of interest, check out our safe-space physician-only FREE peer-support groups.
