So there I was, first day as a shiny new MD. The day before I was Medical Student Corrigan. Today I was DOCTOR C. My first day as a doctor, and boy was I pleased as punch. This article describes my first 24 hours as a practicing physician and focuses on trauma in medicine.
Trigger warning: contains scenes of surgical and emotional trauma.
“Welcome to the Trauma Surgery Unit” said Prof. “As it’s New Year’s Day we’re expecting a quiet one.” Prof’s sense of irony (i.e. sarcasm) was legendary.
That night (first shift) a young man came in. “Stabbed chest. Resus!” came over the PA system, and everyone moved.
Within minutes it became clear that the patient was bleeding out into his own chest. Litres of blood were being pumped in to no avail. His heart stopped. Young and fit, there was still a chance to save him if we could keep his brain and heart perfused with oxygen-carrying blood.
Prof’s 2nd-in-command decided we needed to “crack his chest”, which he proceeded to do like Grampa carving a turkey.
“You, new boy, get your hand in there and start pumping”.
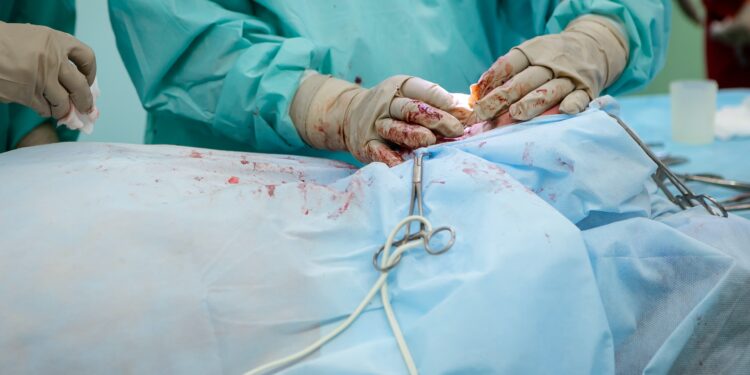
Within 12 hrs of becoming a doctor I had my gloved hand inside a stranger’s chest pumping his now fibrillating heart, while a sweating surgeon swore trying to close a hole in the pulmonary artery.
As I write, it comes back to me like it was yesterday. It was over 2 decades ago.
I can smell the sweet iron of the blood, the nicotine on the surgeon’s breath, the background hospital bleach aroma. The bleeping machines, hushed tones of colleagues, the curses of my boss. The feel of the heart muscle, filling my fist, trembling like a dying fish.
Prof “calling it”. Time of death 19:53.
I looked around. The body still warm, alive mere minutes ago. The surgeon was writing his notes. The nurses were tidying the body. Someone was on the phone notifying the authorities of the death. The bustle continued, but more subdued. The heart monitor kept beeping, searching for a pulse. In vain. No-one switched it off even though it was jarring.
I thought of this young man’s family. His lost potential. His murderer. I was felt sadness started to well up. I just wanted to crawl into a small space and cry it out.
I wanted us to be able to take 5 minutes with a cup of something warm to discuss what just happened.
I doubted we would have time because there was a long line of “minors” that needed seeing to, and only 2 doctors in the unit. Minors were the fortunate majority with injuries unlikely to kill them before we saw them. Broken limbs, glassed faces, head injuries, the drunk and bloodied.
Instead, my beeper went off at the same time as the PA: “GSW abdomen. Resus Bay 2”.
My heart racing, I moved on.
Minors were the fortunate majority with injuries unlikely to kill them before we saw them. Broken limbs, glassed faces, head injuries, the drunk and bloodied.

There are so many more stories I could tell (and one day I might, but I fear they would not be believed).
There’s the case of the patient fallen from his bed whom the nurses refused to pick up because he was a known carjacker. The girl with Down’s Syndrome who died before me of an undiagnosed heart condition. The nice old Greek lady riddled with cancer, unable to eat, but who tried to set me up with her daughter by asking her to bring food in for the “nice doctor”. The patient who suddenly exploded in rage and shouted so aggressively in her face that my psychiatry trainee colleague thought she would be killed. She then lost control of her bladder in front of everyone.
The “attention seeking self-harmer” who no-one took seriously who strangled herself with a bandage alone in the dark on a mental health ward.
Events like this are happening all over the world, probably thousands of times a day. This is just one half a medical career.
Notwithstanding the tragedy of lives lost, human potential cut short, and the evidence of man’s inhumanity to man, there is something else we need to talk about.
They are happening in different settings: intensive care units (think multiple deaths and doctors having to choose between patients for the one available bed during COVID); birthing units (think stuck babies); and in psychiatric wards (think assault by an out-of-control patient or, indeed, relative).
Trauma. In medicine.
Burnout rates are at record highs: before the Pandemic about 43% of doctors were burnt out in the US alone. After nearly 3 years of COVID, the physician burnout rate is 63%.
Just how much exposure to trauma is going on? In one study of 1134 interns, 56% reported trauma exposure during internship, and 19% of those experiencing trauma screened positive for post-traumatic stress disorder.
In another piece of research across many different specialisms, researchers found that one in 5 residents had PTSD (20%) — which remains more than 3 times that of the general population.
Burnout rates are at record highs: before the Pandemic about 43% of doctors were burnt out in the US alone. After nearly 3 years of COVID, the physician burnout rate is 63%.
Resident physicians (also known as trainees, interns, registrars; during their first 4–6 years after medical school) are at highest risk for traumatic exposure. Ironic because these doctors typically have the greatest responsibility for frontline clinical care with high patient volumes, but they lack the training and experience of more senior physicians to deal with the trauma.
So what, you may ask? You wanted to go into medicine, you’re well paid, and being a doctor brings numerous advantages. This is all true.
But you should care because mental distress and illness in physicians contributes medical errors, poorer quality of care, and increased healthcare costs.
In one study of pediatric residents, depressed residents made 6.2 times as many medication errors as residents who were not depressed.
The estimated cost of burnout is nearly $5Bn a year, excluding the costs of medial errors, recruitment, and the human suffering in both patients and healers. There are some estimates that recruiting a single physician can cost as much as $1 million.
Most concerningly, an estimated 300–400 doctors die by their own hands in the US alone, with the US having a higher risk of doctor suicide than Europe. A shocking figure. That’s one per day. One medical school class a year of physicians end their own lives every year.
Suicide deaths are 250%-400% higher among female physicians, compared with women in other professions, and 70% higher among male physicians, compared with men in other professions.
Most concerningly, an estimated 300–400 doctors die by their own hands in the US alone. A shocking figure. One medical school class a year of physicians end their own lives every year.
We need to talk about trauma in medicine. In need to have a lie-down after writing about these harrowing memories.
In future articles, I would like to talk about solutions. In the meanwhile, I’d be very grateful for your feedback.
Thanks so much for reading.
DC
