
If there’s one good thing about a pandemic, it’s increased public awareness of their healthcare workers as human beings under stress. Healthcare organizations, too, are raising the profile of physician wellbeing and putting strategies into place to “care for the carers”. In this article, we have pulled together a number of resources for physician resilience developed by professional organizations for the interested physician reader and physician leader.
If there's one good thing about a pandemic, it's increased public awareness of their healthcare workers as human beings under stress.
Don Berwick’s 2008 Triple Aim model for optimizing health system performance proposed that health care institutions simultaneously pursue 3 dimensions of performance:
In subsequent years, it became clear that a fourth Aim was missing:
4. Care of the care providers.
This Quadruple Aim (Bodenheimer and Sinsky, 2014) made explicit that care team wellbeing was a prerequisite for achieving the Triple Aim.
Ironically, in an effort to achieve the Triple Aim, health care organizations may increase burnout through unintended consequences designed to improve patient care.
Bodenheimer and Sinsky suggest a number of practical steps (with a focus on US Primary Care, but relevant across medicine and globally) for health care organizations to improve the work-life of clinicians and staff. These resources for physician resilience include:
Implement team documentation: all clinical staff can enter some or all documentation into the EHR, assisting with order entry, prescription processing, and charge capture. Team documentation has been associated with greater physician and staff satisfaction, improved revenues, and the capacity of the team to manage a larger panel of patients while going home earlier.
Use pre-visit planning and pre-appointment laboratory testing to reduce time wasted on the review and follow-up of laboratory results
Expand roles, allowing nurses and medical assistants to assume responsibility for preventive care and chronic care health coaching under physician-written standing orders
Standardize and synchronize workflows for prescription refills, an approach that can save physicians 5 hours per week while providing better care
Co-locate teams so that physicians work in the same space as their team members; this has been shown to increase efficiency and save 30 minutes of physician time per day
To avoid shifting burnout from physicians to practice staff, ensure that staff who assume new responsibilities are well-trained and understand that they are contributing to the health of their patients and that unnecessary work is re-engineered out of the practice
These are largely design, engineering, and workflow improvements that tackle inefficiency and our number one bugbear – Electronic Health Records.
However, notably, the authors remind us of the need for investment in primary care in order to address the” chasm between society’s expectations and primary care’s capacity”.
...the need for investment in primary care in order to address the 'chasm between society’s expectations and primary care’s capacity'
Stanford University has developed the excellent Stanford Model of Professional Fulfillment ™. This model consists of 3 dimensions that recognize structural as well as personal factors in physician resilience:
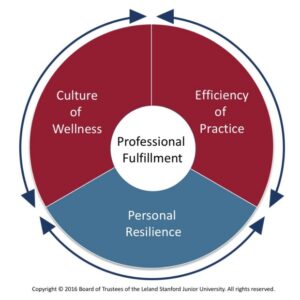
https://wellmd.stanford.edu/about/model-external.html
Key success factors include:
While the organization is responsible for the majority of factors related to well-being, the individual still plays a critical role. Personal Resilience refers to the individual skills, behaviors, and attitudes that contribute to physical, emotional, and professional well-being.
Key success factors include:
So, a number of world-leading organizations have developed resources for physician resilience and programs to help physicians cope better. We hope that many of these will be very helpful.
Certainly, check these out. Learn new ways of coping. Be able to bend with the hurricane rather than break. Become stronger. We hope that by sharing these resources for physician resilience you will benefit.
Please don’t burn out, or worse.
If you need more, though, please check out our Forums and Support Groups – all completely confidential, anonymous, and secure.
If you know of resources that we have left out, please get in contact!
