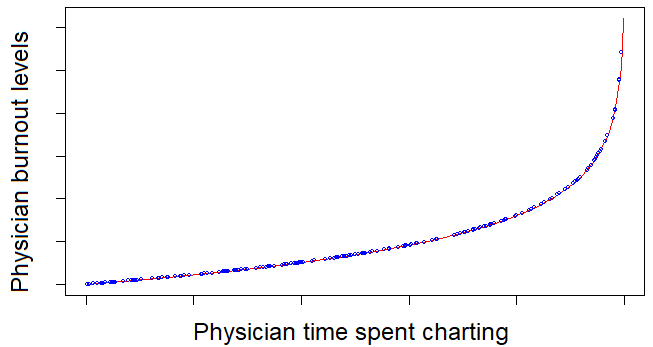
Introduction to physician coaching for burnout prevention
As a psychiatrist, it took me only a few years in practice to realise that everyone needs a therapist (at least once in their lives). Doctors, nurses, and all healthcare practitioners (HCPs) are no different.