
The hidden epidemic: Physicians who stay but mentally quit
Many physicians stay in their roles but have quietly “quit” in spirit—going through the motions while their passion and engagement vanish.

Many physicians stay in their roles but have quietly “quit” in spirit—going through the motions while their passion and engagement vanish.

Let me confess something that might sound ridiculous coming from a doctor: for most of my career, I treated rest like a threat. A sign of weakness. A guilty pleasure to be earned only after I’d answered every email, seen every patient, signed off every note, and probably rotated the tires on someone else’s car just to be safe.

Is the motive behind resilience training to retain staff so that the system can continue to stay revenue-positive, or is it an investment in the ultimate resource of medicine, the human one?

I am just a physician who has spent 20+ years in the ER, had a few leadership roles along the way (which makes for a mildly robust LinkedIn profile), and nurtured some wisdom too. I think that is enough.

After burning out, I learned that chasing a perfect 50/50 work-life balance is unrealistic—especially in medicine. Instead, I now embrace asymmetric balance, where some days work wins, and others, life does.

Psychological safety, defined as a shared belief that the team is safe for interpersonal risk-taking, is a critical component of effective healthcare delivery. Yet, numerous reports and studies indicate that a lack of psychological safety persists in many healthcare settings, leading to adverse outcomes for both patients and providers.

As a psychiatrist, it took me only a few years in practice to realise that everyone needs a therapist (at least once in their lives). Doctors, nurses, and all healthcare practitioners (HCPs) are no different.

At a recent Physicians Anonymous meeting, we discussed an article on random acts of kindness. Researchers gave 84 random people in a wintry Chicago park free hot chocolates. They were then given the choice to gift it to another or keep it for themselves. Guess what happened?

Women physicians still face disproportionate challenges within their medical careers compared to men. Unsurprisingly, those women who face more work-related stressors report less satisfaction with their careers, and more burnout occurs in female doctors.

This blog explores the science of gratitude for physicians, how it may tackle burnout, and gives some suggestions for gratitude practice.

In a previous article, we explored the evidence base for gratitude. In this article, we illustrate 7 physician gratitude practices that may help on a level. We also note that no one intervention is a panacea for the core systemic issues causing the current epidemic of physician burnout and moral injury.

If there is anything positive to come from this pandemic, it is the realization of the importance of peer support. Physician peer support programs with an emphasis on preventing burnout and growing community have are being piloted and implemented in different ways and organizations around the country.

In this article, I write about 5 steps towards physician post-traumatic growth. These are simple daily practices that may help you rebuild with precious metal holding and enhancing your imperfections.

For those of us who survive the trauma of medicine, there is indeed the possibility of physicians rebuilding happier, stronger, maybe even smarter. Like a shattered vase repaired with gold running through it, post-traumatic growth for physicians is a thing.

While traits like conscientiousness, agreeableness, neuroticism are helpful in being a successful and safe clinician, they can have their downsides.

Physician loneliness is a thing. In Part 2, I look at the lonely physician and systemic (“Them”) factors and solutions.
We humans are wired for connection. Our ancestors evolved as social beings because, simply, working together as a band of humanoids increased their chances of survival and reproduction. Multiple studies have shown that collaboration engenders survival advantage. Yet physician loneliness is a real thing.
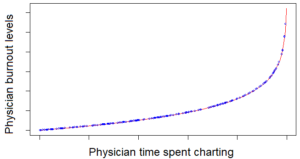
In this article, we look at the connection between charting and physician burnout. We also examine innovations to try and reduce charting-related fatigue and physician burnout.

In this article, we explore the link between the burnout syndrome as it relates to doctors, and the impacts on their physical and mental health.

In this article, we explore the history of the “burnout syndrome” in general and as it relates to physicians specifically. Why is physician burnout history important?

Reach out to your loved ones, and be honest. Trust me, they will help you. You are loved in more ways than you can imagine, because you are one unique lovable bright spot in this world. So stay with us and shine on us. This a Physicians Anonymous co-founder’s story of how she lost a spouse to suicide.