
Hero’s journey: Letting go of self-hate & choosing love instead
One of the biggest lessons I’ve learned on my Hero’s Journey is the importance of learning to accept ourselves (our full selves).

One of the biggest lessons I’ve learned on my Hero’s Journey is the importance of learning to accept ourselves (our full selves).

There has never been a more urgent need to combat, or ideally prevent, physician burnout, mental illness, and suicide. In this article, we explore a number of peer support programs and summarize the key elements required to develop safe and supportive spaces for the unique needs of physicians at risk of burning out.

When you allow yourself to truly see and sit with the fact that we are only here for a short period of time, it can feel scary… and also freeing.

Motherhood is by far the hardest thing that I have ever done and continue doing every day. It is 1 million times harder than being a doctor and requires such a delicate dance of unconditional love, consistency, and compromise. At the same time, there is no doubt that being a physician is one of the hardest professions out there.

I do my best thinking in the quiet, calmness of nature – with space to breathe and observe the beauty of the world around us. I perform best when I have time to think, process, and move at ease with intention. For years, I pushed myself to move faster – with an urgency that was getting me places faster- only to realize I was missing the opportunity to enjoy the journey and the destinations were not where I wanted to be.

Medical residents’ mental health deteriorates during their training, but there are solutions to this resident burnout epidemic.

Few of us swear by Apollo the physician, and Asclepius, and Hygieia and Panacea. But all of us know, “First do no harm,” (which is actually a misquote from the Hippocratic Oath). The Oath underpins much of modern medical ethics and professionalism. Most of us ascribe to these broad principles, but in conversations with distressed colleagues, it is apparent that there are a minority of us who seem to be mired in hypocrisy rather than Hippocrates.

Physician self care is not selfish. It’s essential to thriving in medicine. This article will explore barriers to physician self care and help physicians develop self-care practices for their physical, emotional, spiritual and intellectual health.

When things go wrong, it is easy to focus only on the “first victim” and forget those around them affected by the error – especially the clinician who made a mistake, also known as the “second victim” in medicine.

Physicians Anonymous humbly hosts this living document of global resources for physician support.
Search: Scroll down to your country or press Ctrl+F and enter your keyword to search.
If you would like to add resources or your country please Contact us or leave details in the comments below.

Cognitive distortions are exaggerated or irrational thoughts that we have. In Part 2 of this article, by learning to tackle common cognitive distortions, you will be empowered to manage your amazing mind and smooth over the bumps in the road of a career in medicine.

Extreme stress tends to bring out more of these cognitive distortions, and modern medicine is a rich source of stress for doctors and medical students. We give 6 examples of classic cognitive distortions as applied to medicine, and discover ways to challenge them with more realistic thinking.

T’was the night before Christmas, and all through the ER, everyone was stirring, shouting, vomiting, and hemorrhaging. Except for the mice, who very sensibly stayed away, because it was chaos.

This article explores why residents are at even higher risk of burnout and mental health deterioration than the average physician population. We then look at the evidence base for resident burnout prevention programs and consider why postgraduate education providers should seriously consider investing in these. Mindfulness and Coaching programs are examined as having the most evidence-base.

I recently decided I was going to leave my role as an Emergency Medicine (ER) doctor in the UK National Health Service (NHS). As service after service reaches its full capacity and beyond, the people who rely on these services do not know where to go for the help they need. All of these factors led me do decide that I no longer wanted to commit my daily energies to a system that was causing me to burn out.

A Physician’s Anonymous coach shares 7 days of their physician’s burnout diary, moving from resistance to connection and finding self.

If there was one thing that helped me deal with my own burnout, it was hearing another General Practitioner (GP) stand up in front of a lecture theatre of 200 people and say that they had been burned out too.
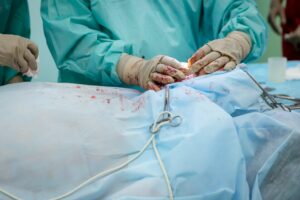
“Welcome to the Trauma Surgery Unit” said Prof. “As it’s New Year’s Day we’re expecting a quiet one.” Prof’s sense of irony (i.e. sarcasm) was legendary. That night (first shift) a young man came in. “Stabbed chest. Resus!” came over the PA system, and everyone moved.

You should know: shame is a very, very bad master. And shame does not deserve your respect, because shame is a liar. Shame is also a huge problem in medicine.

In Part 1, we made the case that a career in modern medicine meets the diagnostic criteria for addiction. Medicine can be unhealthy, yet we carry on or feel unable to make healthy changes. In Part 2, we explore how to get sober if you’re addicted to medicine.

Are physicians addicted to medicine? in this article I will argue that medicine can be so intoxicating, even if it’s bad for us, that doctors can become addicted to it. Before too long, a medical life becomes a way of life until we don’t know any different.